Osteoarthritis
Osteoarthritis is a condition in which the normal smooth articular cartilage lining of a joint is worn down to expose the underlying bone surfaces.
The articular cartilage in a joint is similar to a tyre on a wheel rim- where it acts as a cushion and shock absorber to protect the underlying bone and improve function of the joint.
In osteoarthritis the cartilage is worn away exposing the underlying bone surfaces to abnormal stress. This can lead to pain, inflammation, swelling, a change in the shape and appearance of a joint and limb and stiffness.
In the knee the medial compartment, lateral compartment and patellofemoral compartment can be affected individually or in combination.
Causes
The most common cause of osteoarthritis is primary with a gradual degeneration of the articular cartilage with time: "wear and tear".
Other causes of osteoarthritis are secondary such as trauma, infection, auto-immune conditions and childhood joint pathology.
Symptoms
The most common symptoms patients suffer from are pain, swelling, stiffness, reduced range of motion, and in some cases a change in the appearance, shape and length of the limb.
The pain may occur at rest and if present at night can disturb sleep. The pain may be worsened by daily activities such as walking or hobbies such as gardening or exercise which involve deep bending and twisting of the knee.
Treatment
The management of osteoarthritis is multidisciplinary includes a number of non-operative treatments before proceeding to operative treatments.
Non-operative
These include modifying activities which make the pain worse (eg walking shorter distances at a time, altering exercise regimes to reduce pain), weight loss, using walking aids, and using appropriate painkillers.
Injection treatments
In cases of acute inflammation of the osteoarthritic knee (an increase in pain and swelling) a corticosteroid injection can be performed.
In cases or early articular cartilage wear a PRP (platelet rich plasma) injection may help relieve pain.
Operative
In cases where the non-operative measures have failed there are surgical treatments including arthroscopy, realignment (osteotomy), and joint replacement.
Arthroscopy
Knee arthroscopy is a keyhole procedure which allows visualisation inside the knee and treatment of small cartilage defects and tears of the menisci.
A knee arthroscopy will not change or slow down the arthritic condition of the knee.
It may be useful in patients who have suffered an suspected acute tear of the meniscus in an arthritic knee or for removal of loose cartilage that is causing symptoms in the knee.
Some patients may suffers some worsening of their symptoms after an arthroscopy.
Realignment (osteotomy)
In patients under 55 years of age with osteoarthritis affecting one compartment of the knee, a surgical option is to realign the femur or tibia in order to offload the arthritic compartment of the knee.
Joint replacement
A knee replacement involves removing the damaged cartilage together with small amount of the underlying bone to create flat joint surfaces, perpendicular to the weight bearing axis of the knee, onto which cobalt-chrome knee shaped components are cemented into place.
A plastic (highly cross linked polyethylene) insert is placed as the bearing surface between the two metal components.
If the articular cartilage on the back of the kneecap (patella) is damaged the patella may be resurfaced with a plastic (highly cross linked polyethylene) button or if the articular cartilage is well preserved any bony prominences are excised and a denervectomy of the patella is performed.
In cases of single compartment disease a partial, unicompartmental knee replacement can be performed.
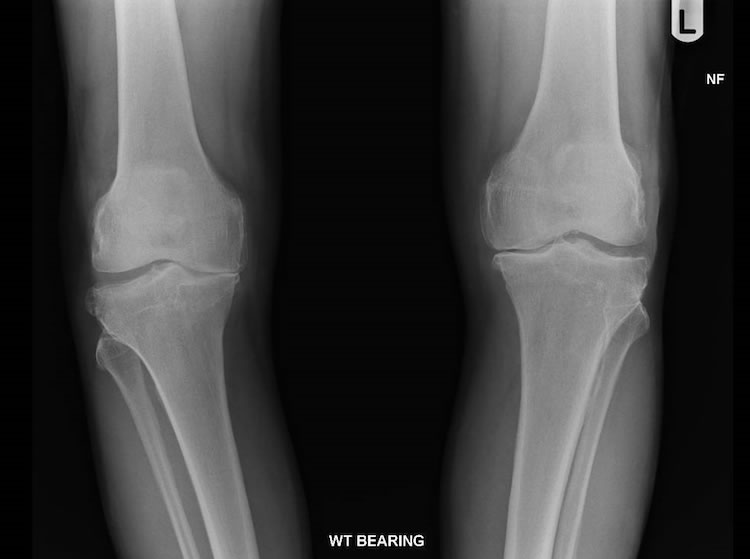
AP radiograph of both knees demonstrating medial compartment articular cartilage loss with marginal osteophytes and lateral osteophytes. Note there is bilateral virus deformity due to the loss of joint space in the medial compartment.